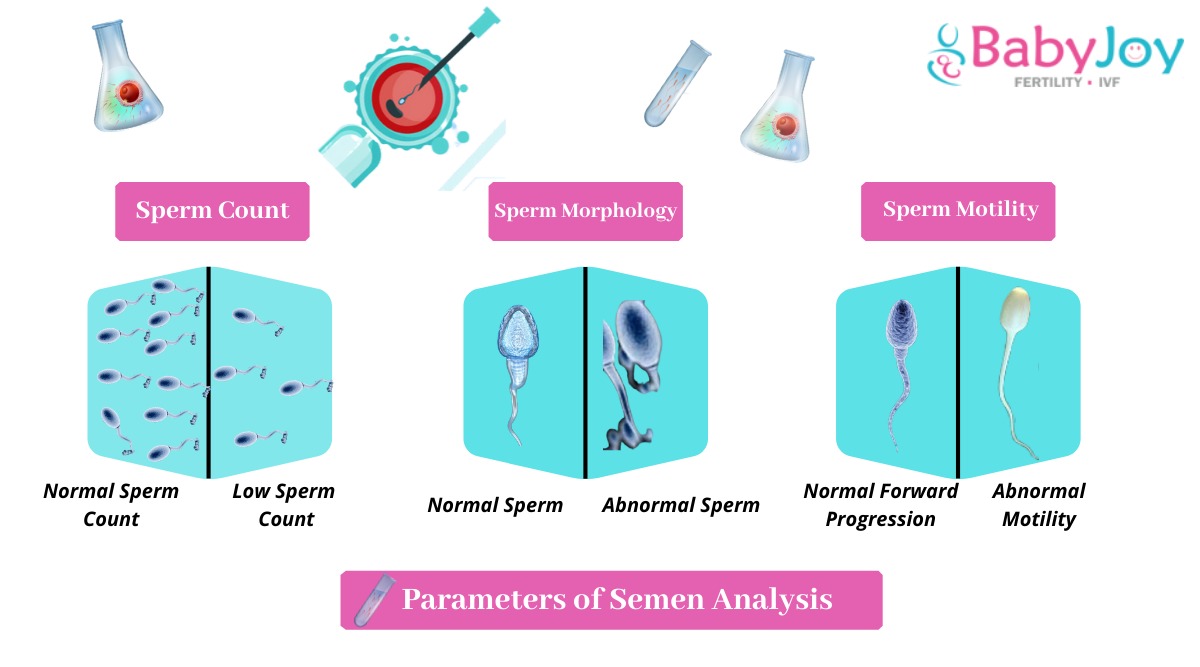
Parameters Of Semen Analysis & Reducing IVF Cost in Delhi
Semen analysis is a technique of examining the fertility of sperm. Also known as Spermiogram, this technique assesses the two components of semen, namely fluid and sperm, to determine the fertility rate of men. It is gaining importance because of the increasing awareness of people regarding the impact of semen on fertility. Proper & timely semen analysis can reduce IVF Cost in Delhi
Various parameters are used by laboratory technicians all over the world for semen analysis. The World Health Organization periodically publishes reference values to measure semen fertility on these parameters. These values are referred to as Lower Reference Limit (LFR).
Volume and Viscosity
Volume refers to the amount of semen ejaculated in one masturbation. According to LFR published by the WHO, a normal male ejaculates 1.5 ml of semen after 3 to 4 days of sexual celibacy. Any amount lower than this is caused either due to physical obstruction in the reproductive tract or because of retrograde ejaculation.
Viscosity is associated with the consistency of semen. It helps in determining any dysfunction in the prostate gland, caused by chronic inflammation. High viscosity decreases the possibility of availability of sperm at the site of fertilization, thus reducing fertility. A gravity-thread test is used to determine the viscosity of semen.

Color and Concentration
One of the basic parameters of analyzing semen is examining its appearance. It can be done at home and requires no special equipment or doctor. Normal semen is opalescent white and slightly yellow in color. Any deviation from this color is an indication of abnormality.
Haematospermia, caused due to the presence of red blood cells in semen, makes it appear brownish in color. The decrease in opacity indicates a lower amount of sperm count. The normal sperm count is supposed to be 15 million per ml ejaculated or 39 million per complete semen sample or more. The lower concentration in sperm count leads to Oligozoospermia.
Motility
The efficiency of sperm movement is known as its motility. The motility of sperm is determined by the percentage of motile and progressively motile spermatozoa. 40% or more motility and 32% or more progressive motility is considered normal. Lower percentage than this is the result of Astenozoospermia.
A sample of 100 spermatozoa is graded into four categories, based on motility: slow or sluggish progressive motility, rapid progressive motility, non-progressive motility, and immotility. A spermatozoon covering a distance of 20 micrometers per second is considered rapidly progressive. The experiment should be carried out at room temperature, between 18 to 24 degrees Celsius.
Morphology
The morphology of the sperm is related to the physical structure of spermatozoa. A spermatozoon is analyzed on the following factors, on the basis of its morphology:
● Shape
A spermatozoon has a head and a tail. The head is the f irst to come in contact with an egg. It releases enzymes to dissolve the outer layer of the egg, making space for the transfer of male chromosomes into the egg.
● Size
The standard size of 5-6 micrometers long and 2.5-3.5 micrometers wide.
The sperm must have a well-defined acrosomal region with 40% to 70% of the head area. A neck, midpiece, tail defects or cytoplasmic droplet more than one-third the size of a normal sperm head must not be present. WHO’s Lower Reference Limit says that at least 4% of the semen sample should have normal morphology.
Takeaway
Many other parameters such as the number of healthy and damaged sperm, coagulation and liquefaction, fructose percentage, pH level, number of immature sperm, amount of leukocytes and the number of infected cells can also be used for semen analysis. The sample should be analyzed within an hour collection for accurate results. There should be a gap of two to three weeks between the study of two samples. Semen analysis helps to chalk out proper Fertility or IVF Treatment & can help in lowering IVF Cost in Delhi. Compromised semen quality calls for IUI/ IVF treatment. However, if semen quality is very poor then IVF-ICSI can be done. This would slightly increase IVF Cost in Delhi, but would yield successful results.


 +91-88-0000-1978
+91-88-0000-1978